Contents |
Branch Retinal Artery Occlusion and Central Retinal Artery Occlusion
Introduction and Overview
We are conditioned to maintain a healthy diet and a healthy lifestyle from every direction; we usually think this is to prevent heart disease, diabetes or stroke. What most of us don’t realize is that what is happening elsewhere in the body is also happening within the eyes.
As we age, a natural plaque begins to form in the arteries that allow the blood to carry nutrients and oxygen to all parts of the body. No one is exempt from this, but it only becomes a problem if the amount of plaque causes loss of elasticity in the artery walls and hardens. Deposits made up of cholesterol, calcium or fatty tissues can eventually break loose and cause a blockage of an artery, especially in the smaller vessels like those found in the eye.
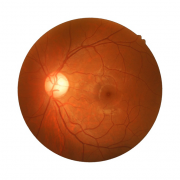
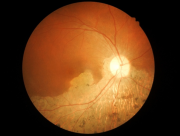
During a comprehensive vision examination, an eyecare practitioner will look at the retina and other structures in the back of the eye for any signs of unusual changes. It is fascinating to think that what is happening in the body in general is usually reflected in the eye, especially changes in the circulatory system. The eye is the one place where the arteries and veins may be seen directly without cutting anything open, an advantage few of us stop to realize.
When a retinal artery is blocked, it is known as a Central Retinal Artery Occlusion (CRAO), or if it affects only a branch of the artery, a Branch Retinal Artery Occlusion (BRAO). The only difference between the two is the location of the blockage of circulation. Where a branch occlusion may affect only a part of the visual field, a central occlusion can affect the entire retina, but otherwise the risk factors and prognosis are the same.
Risk factors for developing hardening and plaque formation in the arteries include:
- Family history of hardening arteries (arteriosclerosis)
- Family history of plaque formation in the arteries (atherosclerosis)
- Smoking
- High cholesterol, or an unfavorable ratio of “good” to “bad” cholesterol
- Hypertension (high blood pressure)
- Diabetes
- Family history of high cholesterol and/or stroke
- History of intravenous drug use
- History of carotid artery disease
- History of heart rhythm problems or generalized heart disease
When plaque builds up in the arteries, there is the potential for pieces to break loose from the artery walls and float down the artery much like a log raft in a river. When such * debris encounters a narrowed place where the walls have hardened, or perhaps in a place where the artery forks into two branches, the log raft can jam and stop the circulation from reaching the areas served by that artery further along.
Ocular Complications
Another way to think of a BRAO or CRAO is that is it like a mini-stroke, where instead of interrupting the blood flow to the brain, part of the retina has been affected instead. The result can be damage to the retina and vision loss.
A blood clot or embolism forms when debris originating from the carotid artery or sometimes, from the heart itself, can block blood flow into the eye and can affect the entire eye or just a part of it, depending on where the clot forms. The area of the retina (the layer of nerve fibers that transmit light signal to the brain) that is no longer receiving oxygen or nutrients can be permanently damaged very quickly, resulting in a loss of vision.
Even when the duration of circulation loss is very short, damage to the retina may result in profound and permanent vision loss.
Patients who experience a BRAO or CRAO may experience severely blurred vision and light and colors may seem much dimmer in one eye, especially when compared to the other. Some people report a sense of having a shade or curtain that is covering part of their vision.
Retinal artery occlusions are always an ocular emergency; it is essential that medical intervention begins right away, within unfortunately, treatment options for BRAOs are few and not usually completely successful. Unless the occlusion can be diagnosed and treated within the first one to two hours; some vision loss is likely in most cases.
Treatment
Symptoms of a BRAO or CRAO should be reported to an eyecare practitioner immediately. The most common symptoms are either a sudden blurriness or loss of vision in one eye, especially in someone who has any of the other risk factors listed above.
In order to assess where the blockage is located and the extent of possible damage tests such as flourescein angiography, where a fluorescent dye is injected into a vein and a sequence of photographs are taken with ultraviolet-sensitive film may be performed. Flourescein angiography is also used to assess the presence and extent of retinal neovascularization later in the course of the disease.
There is no generally agreed-upon treatment regimen, but there are several steps which if taken in the very early stages of the occlusion, may prevent irreversible loss of vision.
- Within 90 to 180 minutes of onset of symptoms, ocular massage may be attempted to dislodge the blockage.
- Reduction of intraocular pressure in an attempt to increase arterial blood flow.
- “Clot-busting” drugs such as those that might be used after a stroke, also in an attempt to increase arterial blood flow to the affected area.
- For the long term, medications the reduce blood clotting such as low-dose aspirin may be indicated.
In the long term, the prognosis for the recovery of vision in the affected eye is poor; only about a third of patients show any improvement of the vision. Some people do experience a spontaneous resolution of the blockage. In a lucky few, spontaneous resolution of the blockage occurs, but this is seen in only about 8 to 12% of patients experiencing BRAO. Reduced circulation in the eye such as that seen in BRAO, diabetic retinopathy or proliferative macular degeneration can often lead to the growth of new arterial blood vessels in the eye, which are extremely fragile and may break and leak blood into the eye. It is essential to monitor the retina on a regular basis for any sign of these changes. Treatment for neovascularization is laser photocoagulation, which seals off the new vessels.
Because of the risk for systemic cardiovascular and coronary disease, patients with a retinal artery occlusion should be evaluated to assess their cardiovascular health and be monitored closely. It is appropriate that they should have more proactive care as well, including blood pressure and lipids to prevent future heart disease.
Summary
Eyecare practitioners and primary care physicians should be aware that patients who are at risk for BRAO or CRAO may also present with other circulatory complications, including temporal arteritis and stroke.
The prognosis for recovery of useful vision in the affected area is poor, but further loss may be prevented by systemic treatment of hypertension, heart disease, carotid artery disease, diabetes, and a strong warning to patients who smoke to stop doing so as soon as possible.
On the positive side, however, doctors are investigating laser surgery to help rectify retinal damage and visual impairment caused by the occlusion of the retinal arteries.
Diet, exercise and a generally healthy lifestyle are probably the best preventive measures that can be taken, as we are almost always reminded.