Contents |
Glaucoma: Is it Possible to Prevent Vision Loss?
Introduction
According to a study done in 2004 at The Ohio State University, it might be, for certain individuals in certain circumstances.
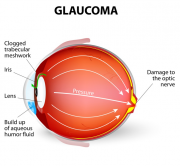
Glaucoma is a group of diseases usually characterized by higher than normal pressures within the eye; the increased pressure can compress the retinal nerve fibers, particularly where they come together and form the head of the optic nerve, located in the back of the eye. The most common type of the condition, primary open-angle glaucoma, was the subject of the study.
Eyecare professionals have estimated that at least half of all glaucoma patients don’t know they have the disease, because it has no symptoms until quite advanced. Glaucoma causes damage to the peripheral vision first, and many people don’t notice that their field of view has gradually begun to shrink. The increased pressure within the eye almost never produces pain, for example, or noticeable vision changes in its early stages. If left untreated, however, it is one of the leading causes of functional blindness. The increased pressure damages and eventually causes the nerve fibers of the retina to become compressed and die; vision loss from glaucoma is permanent. For this reason, it is important to diagnose and begin treatment early in the disease process to prevent vision loss.
Glaucoma is a complex condition, however, and patients are not automatically classified as having glaucoma if the pressure in the eye higher than normal, if there is no other sign of disease or damage present.
This particular study targeted people of African descent, because their risk for developing early glaucoma is higher. In fact, people of African descent are three times as likely to acquire glaucoma, and generally the disease has an earlier onset in this population.
The Study
The study, published in Archives of Ophthalmology, enrolled about 1600 patients who had elevated "intraocular pressure (IOP)" readings, but no damage to the ocular tissues as measured by standardized testing equipment and visual inspection of the nerve head. The study group included 408 people of African descent.
Half of the subjects/patients were given commercially available, physician-prescribed eye drops used to lower IOP in the treatment of glaucoma and asked to use them each day. (Although the study was supported by Merck Research Laboratories, there was no restriction on the type or brand of eye drops prescribed for any individual.) The other half of the patients were given no eye drops or other medical treatment. Both groups were followed carefully for several years to assess any possible damage these higher IOPs may be causing.
Results
Patients enrolled in the study that were given pressure-lowering eye drops went on to develop glaucoma at a rate of about 8.5%, while those without medical intervention developed glaucomatous damage at just over 16%, almost twice as often. This effect was especially noticeable in the group of African-descent individuals.
This does not necessarily mean, however, that all people with moderately high IOPs or all people of African descent should automatically be placed on glaucoma medication. The most popular and useful pressure-lowering eye drops are considered to be safe and effective, but they are not without side effects or expense.
Dr. Eve Higginbotham, chair of the University of Maryland Medical Center’s Department of Ophthalmology, and a co-author of the study, said that extent of damage and the patient’s general health are among other factors to consider when contemplating treatment.
However, in practical terms, it does mean that everyone, regardless of ethnic background should have regular eye examinations. Many people have the idea that as long as their vision seems normal and they are experiencing no pain, headaches or other symptoms that they don’t need their eyes checked, but glaucoma is more insidious and sneakier than most other conditions or diseases. Only a qualified eyecare practitioner can diagnose and treat glaucoma.